A síndroma de Terson é caracterizada pela presença de hemorragia intraocular, secundária a uma hemorragia subaracnoideia (mais comum) ou subdural. Há várias hipóteses para explicar este facto. Aceita-se geralmente que o fluido no compartimento intracraniano extravascular provoca um aumento da pressão intracraniana que consequentemente leva a um aumento da pressão intraluminal nos canais venosos que drenam o globo ocular. Por sua vez, este aumento conduz a uma rotura das veias intraoculares e hemorragia.
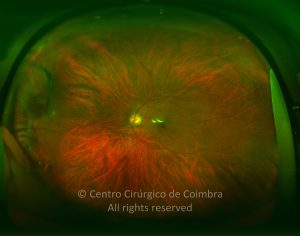
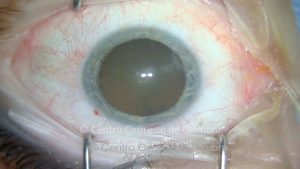
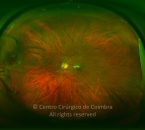
A hemorragia pode ser subretiniana, intrarretiniana, prerretiniana (sub-hialóide) ou intravítrea. Da hemorragia pode também resultar um quisto macular hemorrágico (CMH). O CMH está presente em mais de 40% dos doentes com síndroma de Terson. Têm sido descritos dois tipos de CMH. O CMH submembranoso, com sangue acumulado sob a MLI, e no CMH prerretiniano, com sangue localizado entre a MLI e a hialoideia posterior. O quisto pode ter diversas aparências de acordo com a idade. Inicialmente é vermelho, tornando-se branco com a reabsorção do sangue, e transparente quando a sua reabsorção é completa.
A hemorragia intraocular, no contexto da hemorragia intracraniana, tem implicações no prognóstico. Nos doentes com hemorragia subaracnoideia e síndroma de Terson, a mortalidade é duas vezes maior do que em doentes com hemorragia intraocular. O risco de coma num doente com hemorragia intracraniana e síndroma de Terson duplica quando comparado com os casos que não têm hemorragia intraocular. Por este motivo, o exame dos doentes com hemorragia subaracnoideia ou subdural sob midríase é obrigatório.